Psoriasis is more than just a skin condition—it’s a chronic autoimmune disorder that can affect your daily life, confidence, and overall health. If you or someone you care about is dealing with psoriasis, understanding its symptoms and available treatments is essential.
In this comprehensive guide, we’ll walk you through everything you need to know about psoriasis, including what causes it, how it manifests, and most importantly, how to manage it effectively. This article is written for easy readability, follows Google AdSense content policies, and is fully SEO-optimized.
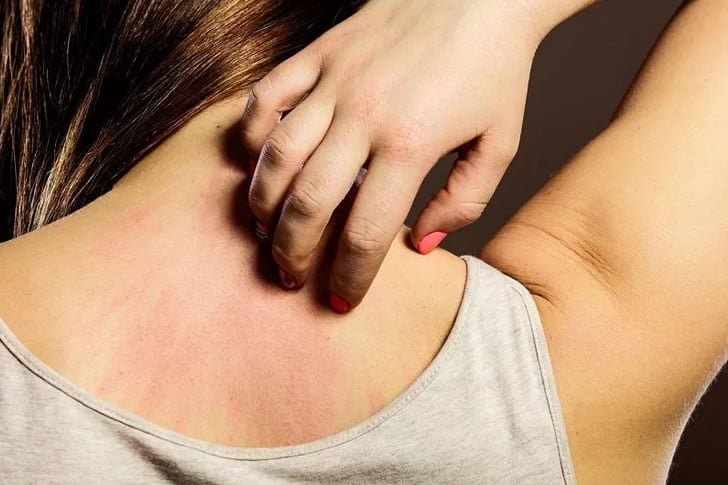
What is Psoriasis?
Psoriasis is a long-lasting autoimmune skin condition that causes the body to produce new skin cells too quickly. Instead of taking weeks, new skin cells form in just days. This leads to a buildup of skin cells on the surface, resulting in thick, scaly patches.
It is not contagious, but it can be lifelong, with periods of flare-ups and remission.
Common Symptoms of Psoriasis
The symptoms can vary based on the type of psoriasis, but common signs include:
- Red patches of skin covered with silvery-white scales
- Dry, cracked skin that may bleed
- Itching, burning, or soreness
- Thickened or ridged nails
- Painful, swollen joints (in psoriatic arthritis)
These symptoms may appear on the:
- Scalp
- Elbows
- Knees
- Lower back
- Palms and soles
- Face and genitals (in rare cases)
Types of Psoriasis
There are several types of psoriasis, each with unique symptoms:
1. Plaque Psoriasis (Psoriasis Vulgaris)
This is the most common form, affecting 80–90% of people with the condition.
2. Guttate Psoriasis
Often seen in children or young adults, it causes small, drop-shaped sores on the arms, legs, and trunk.
3. Inverse Psoriasis
Red, shiny patches that appear in skin folds (armpits, groin, under breasts).
4. Pustular Psoriasis
Characterized by white, pus-filled blisters surrounded by red skin.
5. Erythrodermic Psoriasis
A severe and rare form, causing intense redness and peeling over much of the body. It may require immediate medical attention.
What Causes Psoriasis?
Psoriasis is an autoimmune disorder, meaning the immune system mistakenly attacks healthy skin cells.
Possible Triggers:
- Stress
- Skin injuries (cuts, scrapes, sunburns)
- Infections (like strep throat)
- Certain medications (lithium, beta-blockers)
- Cold, dry weather
- Smoking and alcohol use
Genetics also play a significant role. If someone in your family has psoriasis, your chances of developing it increase.
How is Psoriasis Diagnosed?
A dermatologist typically diagnoses psoriasis by:
- Examining your skin, scalp, and nails
- Asking about your symptoms and medical history
- In rare cases, performing a skin biopsy to rule out other conditions
Effective Treatments for Psoriasis
While there’s currently no cure, many treatments can help manage the symptoms and improve the quality of life.
1. Topical Treatments
These are applied directly to the skin and are typically the first line of defense.
- Corticosteroids: Reduce inflammation and itching.
- Vitamin D analogs: Slow skin cell growth.
- Coal tar: Reduces scaling, itching, and inflammation.
- Moisturizers: Prevent dryness and cracking.
2. Phototherapy (Light Therapy)
Exposing the skin to ultraviolet (UVB) light under medical supervision can reduce flare-ups.
- Narrowband UVB therapy: Common and effective.
- PUVA therapy: Combines UVA light with a medication called psoralen.
3. Systemic Treatments (Oral or Injectable)
These are for severe or treatment-resistant psoriasis.
- Methotrexate
- Cyclosporine
- Biologics like adalimumab, etanercept, or secukinumab, which target specific parts of the immune system
4. Over-the-Counter (OTC) Products
OTC creams containing salicylic acid, coal tar, or hydrocortisone may help mild cases.
Lifestyle Tips for Managing Psoriasis
In addition to medical treatment, lifestyle changes can greatly reduce flare-ups:
1. Maintain Skin Moisture
- Use fragrance-free moisturizers
- Apply after bathing to lock in moisture
2. Manage Stress
Stress is a known trigger. Try relaxation techniques such as:
- Yoga
- Meditation
- Deep breathing exercises
3. Avoid Triggers
Identify and avoid things that make your symptoms worse, like alcohol, spicy foods, or smoking.
4. Take Care of Your Scalp
If psoriasis affects your scalp:
- Use medicated shampoos with coal tar or salicylic acid
- Avoid scratching to prevent infections
5. Follow a Healthy Diet
Some people notice improvement with an anti-inflammatory diet rich in:
- Omega-3 fatty acids (salmon, flaxseeds)
- Vegetables and fruits
- Whole grains
Psoriasis in Children
Children can also develop psoriasis. It may be harder to diagnose because it can mimic other skin conditions like eczema. Pediatric psoriasis usually appears as plaque psoriasis and is managed with gentle topical treatments.
Psoriatic Arthritis
Up to 30% of people with psoriasis develop psoriatic arthritis, a condition that affects joints. Symptoms include:
- Stiff, painful joints
- Swollen fingers and toes
- Morning stiffness
It’s important to catch it early to prevent joint damage.
When to See a Doctor
You should see a dermatologist if:
- Your symptoms are worsening
- Over-the-counter treatments don’t work
- You notice joint pain or stiffness
- Your quality of life is affected
Psoriasis and Mental Health
Living with a chronic condition like psoriasis can affect your mental well-being. Many patients experience:
- Anxiety
- Depression
- Social withdrawal
Talking to a therapist and joining support groups can provide emotional support and coping tools.
Common Myths About Psoriasis
Myth 1: Psoriasis is contagious – False. It’s an autoimmune condition, not an infection.
Myth 2: Only adults get psoriasis – False. Children can also develop it.
Myth 3: Psoriasis is just dry skin – False. It involves an immune system response and needs proper treatment.
Conclusion
Managing psoriasis takes patience and a personalized approach. With the right treatment plan and lifestyle changes, you can keep flare-ups under control and enjoy a better quality of life. Always work closely with a dermatologist to find the treatment that works best for you.
Stay informed, stay proactive, and remember—you’re not alone in this journey.
⚠️ Disclaimer: This article is for informational purposes only. Always consult a licensed healthcare professional for medical advice and diagnosis.